Conditions We Treat- Spinal
TriState Neurological Surgeons, Inc. is Erie Pennsylvania's expert in treatment of Spine Disease. We offer all the latest management options, focusing on conservative and minimally invasive procedures like Microdiscectomy, Kyphoplasty, X-Stop™ and Interventional Pain Management, rather than major surgery whenever feasible.
Our physicians provide compassion combined with knowledge and experience.
Below is a list of the spine conditions we treat:
Back Pain
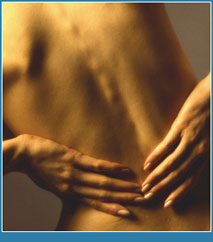 Back pain most commonly involves the low lumbar area and may originate from the muscles, nerves, bones, joints or other structures of the spine. The pain may have a sudden onset or it can be a chronic pain; it can be felt constantly or intermittently, stay in one place or refer or radiate to other areas. It may range from a dull ache to a sharp piercing or burning sensation. The term is used by patients to also describe pain in the lower neck (between the shoulder blades) or the upper back. The term itself then does not indicate or diagnose one problem. Back pain may be associated with other symptoms such as arm or leg pain, and may include symptoms other than pain, such as weakness, numbness or tingling. Back pain is one of humanity's most frequent complaints. In the U.S., acute low back pain (also called lumbago) is the fifth most common reason for all physician visits. About nine out of ten adults experience back pain at some point in their life, and five out of ten working adults have back pain every year.
Back pain most commonly involves the low lumbar area and may originate from the muscles, nerves, bones, joints or other structures of the spine. The pain may have a sudden onset or it can be a chronic pain; it can be felt constantly or intermittently, stay in one place or refer or radiate to other areas. It may range from a dull ache to a sharp piercing or burning sensation. The term is used by patients to also describe pain in the lower neck (between the shoulder blades) or the upper back. The term itself then does not indicate or diagnose one problem. Back pain may be associated with other symptoms such as arm or leg pain, and may include symptoms other than pain, such as weakness, numbness or tingling. Back pain is one of humanity's most frequent complaints. In the U.S., acute low back pain (also called lumbago) is the fifth most common reason for all physician visits. About nine out of ten adults experience back pain at some point in their life, and five out of ten working adults have back pain every year.
The spine is a complex interconnecting network of nerves, joints, muscles, tendons and ligaments, and all are capable of producing pain. Large nerves that originate in the spine and go to the legs and arms can make pain radiate to the extremities.
Back pain can be a sign of a serious medical problem, although this is not most frequently the underlying cause. In general, however, back pain does not usually require immediate medical intervention. The vast majority of episodes of back pain are self-limiting and non-progressive. Most back pain syndromes are due to inflammation, especially in the acute phase, which typically lasts for two weeks to three months. In cases of persistent or disabling back pain, only a thorough physical and neurological exam coupled with diagnostic testing can yield a proper diagnosis.
Cauda Equina Syndrome
Cauda Equina Syndrome is a serious neurologic condition in which there is acute loss of function of the lower extremities as well as bowel and bladder function due to compression of the nerve roots within the lumbar canal. The nerve roots within the lumbar canal find their origin in the termination of the spinal cord and collectively are termed the cauda equina.
Any lesion which compresses or disturbs the function of the cauda equina may disable the nerves although the most common is a large central disc herniation .
Tumors, either originating in the neural structures themselves or metastatic may also give rise to cauda equina syndrome due to compression of the cauda equina by tumor growth or expansion from hemorrhage.
Direct trauma from penetrating injuries or bullet wounds may lead to cauda equina syndrome, Lumbar puncture can also cause cauda equina syndrome. Other trauma-related causes include resulting in posterior migration of fragments of the vertebral body, spinal anesthesia involving trauma from catheters and high local anesthetic concentrations around the cauda equina.
The management of cauda equina syndrome involves rapid diagnosis and frequently involves surgical decompression. MRI of the lumbar spine is most often utilized, but CT scanning may also be utilized.
Cauda equina syndrome of sudden onset is regarded as a medical/surgical emergency. Surgical decompression by means of decompressive lumbar laminectomy or other approaches may be undertaken as soon as feasible if a compressive lesion, e.g. ruptured disc, epidural abscess, tumor or hematoma is demonstrated. This treatment may significantly improve the chance that long-term neurological damage will be avoided. When cauda equina is caused by a herniated disk early surgical decompression is recommended.
The prognosis for complete recovery is dependent upon many factors. The most important of these factors is the severity and duration of compression upon the damaged nerve(s). As a general rule the longer the interval of time before intervention to remove the compression causing nerve damage the greater the damage caused to the nerve(s).
Damage can be so severe and/or prolonged that nerve regrowth is impossible. In such cases the nerve damage will be permanent. In cases where the nerve(s) has been damaged but is still capable of regrowth, recovery time is widely variable. Surgical intervention with decompression of the cauda equina can assist recovery. Delayed or severe nerve damage can mean up to several years' recovery time because nerve growth is exceptionally slow.
Central Cord Syndrome
Central cord syndrome is a clinical presentation of a patient who has complaints of numbness and burning dysesthesthias of the upper extremities, and in particular the hands, combined with weakness of the arms and legs. The arm weakness tends to be more pronounced than the leg weakness. There can be profound abnormalities of the bowel and bladder function, with frank incontinence as well.
Central cord syndrome is seen in the setting of cervical stenosis. Generally the patient has undergone a hyperextension type injury to the cervical spine. A typical story would involve an elderly person striking their forehead or chin on a piece furniture while falling.
Treatment for this condition involves immobilization of the cervical spine with a hard collar, and a radiographic evaluation of the cervical spine. Typically plain Xrays and MRI are performed, by CT scanning may also be undertaken. It is important to rule out any instability of the cervical spine which might have occurred during the hyperextension injury. Ligaments of the spine, as well as discs can be disrupted by this mechanism of injury, as well as the occurrence of bony fractures.
In the absence of instability and fracture, what is usually found on radiographic evaluation is cervical stenosis and spinal cord impingement by bulging discs/spurs and overgrown ligamentum flavum. If an MRI has been performed, thee might be “high signal” within the substance of the spinal cord, indication edema in the spinal cord from the spinal cord injury. Generally, unless the patients neurological status is deteriorating, surgery is not performed in an emergency fashion unless there is severe compression of the spinal cord due to herniated cervical disc or other lesion. Instead time is taken to allow the edema and swelling of the spinal cord to abate, and to assess the patients medical status and ability to undergo surgery, since as stated above, a lot of these patients are elderly. Surgery will ultimately be offered in those individuals who have significant spinal stenosis or compression of the spinal cord. This will relieve the compression of the cord so that continued low grade damage is avoided, and of course avoids an additional central cord injury due to another hyperextension injury. The exact type of surgery offered is influenced significantly by the exact cause of spinal cord compression, how many spinal segments are involved, the preservation or loss of normal cervical lordosis as well as the patients age and medical condition.
The prognosis for patients with a central cord syndrome is guarded. Some may make improvement, but the presence of residual effects from the spinal cord injury is generally the rule. Many patients experience considerable recovery in the first six weeks post injury.
If the underlying cause is edema, recovery may occur relatively soon after an initial phase of motor paralysis or pareses. Leg function usually returns first, followed by bladder control and then arm function. Hand movement and finger dexterity improves last. If the central lesion is caused by hemorrhage or ischemia, then recovery is less likely and the prognosis is more devastating.
The prognosis in younger patients is favorable. Within a short time, a majority of younger patients recover and regain the ability to ambulate and perform daily living activities. However, in elderly patients the prognosis is not as favorable, with or without surgical intervention.
Chiari Malformation
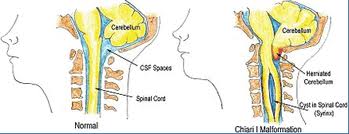
Chiari malformation is considered a congenital condition, although acquired forms of the condition have been diagnosed. This disorder is categorized in order of severity; types I, II, III, and IV. The term "Arnold-Chiari" is applied to the Chiari type II malformation. These malformations, are closely associated with syringomyelia and hydromyelia.
The cerebellum controls the coordination of motion, and is normally located inside the posterior skull, in what is referred to as the posterior fossa. Along the under surface of the cerebellar hemispheres, there are two small protrusions called the tonsils. These structures are located just above the foramen magnum, the largest opening at the base of the skull through which the spinal cord enters and connects to the brainstem.
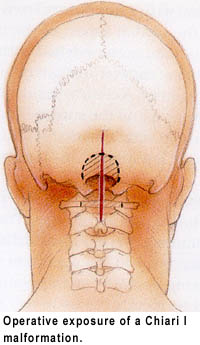
Types of Malformations
Type I Chiari malformation
This malformation occurs during fetal development and is characterized by downward displacement by more than four millimeters, of the cerebellar tonsils beneath the foramen magnum into the cervical spinal canal. This displacement may block the normal pulsations of CSF between the spinal canal and the intracranial space. This form of Chiari malformation may be associated with
syringomyelia.
Anomalies of the base of the skull and spine may also be seen in patients with Chiari I malformation. These possibly include bony abnormalities of the craniocervical junction (spina bifida occulta of arch of Ci, partial fusion of the vertebral arches of C1 and C2, Klippel Feil deformity and basilar impression of the spine resulting in brainstem compression.
Symptoms
Many people with Chiari I malformation have no symptoms. Many individuals complain of severe headaches, possibly associated with neck pain. The headache may be located primarily in the suboccipital area, and may be aggravated by coughing or sneezing. Many other patients complain of weakness of arms and /or legs, difficulty with balance, dizziness and blurred vision. Other symptoms related to a Chiari malformation are due to the development of a syrinx within the spinal cord. these symptoms include loss of pain and temperature sensation of the upper extremities, loss of strength and muscle mass of the hands and upper extremities, spasticity and difficulty with walking.
Type II Chiari malformation
This malformation is characterized by downward displacement of the medulla, fourth ventricle, and cerebellum into the cervical spinal canal, as well as elongation of the pons and fourth ventricle. This type occurs almost exclusively in patients with myelomeningocele.
Type III Chiari malformation
This malformation includes a form of dysraphism with a portion of the cerebellum and/or brainstem pushing out through a defect in the back of the head or neck. These malformations are very rare and are associated with a high early mortality rate, or severe neurological deficits in patients that survive.
Type IV Chiari malformation
This malformation is the most severe form and the rarest. The cerebellum fails to develop normally. There may be other associated malformations of the brain and brainstem. Most babies born with this malformation do not survive infancy.
Treatment
Treatment of Chiari malformations and syringomyelia is very dependent on the exact type of malformation, as well as progression in anatomy changes or symptoms.
Chiari I malformations that are asymptomatic do not require surgery. If the malformation is symptomatic, or the cause of a syrinx, surgical treatment is usually recommended.
The goal of surgery is to relieve the symptoms associate with the Chiari malformation, and stop the progression of an associated syrinx if one is present. Chiari I malformations may be treated surgically with local decompression of the overlying bones and release of the dura (a thick membrane covering the brain and spinal cord). Rarely some degree of cerebellar tissue resection may be performed along with this decompression.
Decompression is performed under general anesthesia. It consists of removing the back of the foramen magnum and often the back of the first few vertebrae to the point where the cerebellar tonsils end. This provides more space for the brainstem, spinal cord, and descended cerebellar components. A tissue graft is often spliced into this opening to provide even more room for the unimpeded passage of CSF. This decompression of the craniocervical junction will allow resolution of the spinal syrinx symptoms in the majority of cases. Occasionally, the syrinx cavity within the spinal cord may be drained with a diverting shunt tube. Chiari II decompression is treated similarly, but is usually restricted to decompressing the tissues in the spinal canal and leaving the back of the skull alone.
Outcome
The benefits of surgery should always be weighed carefully against its risks. Although some patients experience a reduction in their symptoms, there is no guarantee that surgery will help every individual. Nerve damage that has already occurred usually cannot be reversed. Some surgical patients need repeat surgeries, while others may not achieve symptom relief.
Disc Herniation (Herniated Spinal Disc)
A spinal disc herniation, incorrectly called a "slipped disc", is a medical condition affecting the spine, in which a tear develops in the wall of an intervertebral disc and allows the soft, central portion of the disc (nucleus pulposus) to herniate through the wall of the disc (annulus fibrosis). The nucleus pulposus has a very different pH value when compared to the tissues in the spinal canal, and also contain substances called inflammatory mediators. The release of this material of low pH along with it’s inflammatory chemical mediators may directly cause severe pain, even in the absence of nerve root compression. This is the rationale for the use of anti-inflammatory treatments for pain associated with disc herniation, protrusion, bulge, or disc tear.
Disc herniation is commonly seen in the setting of a known disc bulge, a condition in which the outermost layers of the annulus fibrosis are still intact, but can bulge when the disc is under pressure. This bulging is a consequence of the loss of disc material (nucleus pulposus) due to degeneration, as well as some loss of the integrity of the disc wall itself. Some, but certainly not all degenerated discs will herniate, and in fact a disc which is not degenerated will not herniate. Genetics play an important role in determining the risk of a degenerated disc going on to herniation.
Disc herniations can occur from general wear and tear (degeneration), but also maybe related to occupational related injury. This can be seen especially in jobs that require lifting. Traumatic injury to lumbar discs commonly occurs from lifting while bent at the waist, rather than lifting while using the legs. When the spine is straight, such as standing or lying down, internal pressure is equalized on all parts of the discs. While sitting or bending to lift, internal pressure on the disc can move from 17 psi (lying down) to over 300 psi (lifting with a rounded back). This is why proper body mechanics while lifting is so important. With improper lifting technique, the back is rounded which causes the front wall of the lumbar disc to be compressed while the back wall is stretched and under great pressure. This may set the back-side disc wall up for a tear which may allow the nucleus of the disc to herniate through.
Surgery is indicated if a patient has a significant neurological deficit (severe weakness, trouble with bowel/bladder function), or if they fail non-surgical therapy. The surgical procedure for herniated cervical discs include the anterior cervical discectomy and fusion and the posterior foramenotomy and discectomy. Surgical procedures offered for herniated lumbar discs include lumbar microdiscectomy and lumbar minimally invasive discectomy
. The specific procedure chosen by the surgeon depends on the patients anatomy, the pathology present and what approach in the surgeon’s experience is the most efficient solution to the patients problem. In this manner a successful surgery may be tailored to the patients needs.
The presence of cauda equina syndrome (in which there is incontinence, weakness and genital numbness) is considered a medical emergency requiring immediate attention and possibly surgical decompression. A primary focus of surgery is to remove “pressure” or the mechanical compression of the spinal cord or nerve root.
Low Back Sprain and Strain
Lumbar (lower back) muscle strains and sprains are the most common causes of low back pain. The lumbar spine is vulnerable to this type of injury due to its requirement to function as a supporting structure which also must provide significant motion. Muscle strain is caused when muscle fibers are abnormally stretched or torn. Muscle sprain is caused when ligaments are torn from their attachments. When the lumbar spine is strained or sprained, the soft tissues become inflamed. This inflammation causes pain, muscle spasms and significant physical limitations.
Symptoms include overwhelming low back pain which does not radiate into the legs (although it may involve the upper buttocks). Patients usually are bent forward at the waist, and experience increased back pain of they attempt to tighten the abdominal muscles. Patients usually complain of significant back stiffness, and a very limited range of motion of the lumbar spine. This limitation of motion interferes with normal activities of daily living such as putting on clothing (shoes and socks), rolling over in bed or bending to pick up items on the floor). Patients also may experience significant low back muscle spasms.
Treatment
Lumbar sprain and strain is a self limiting condition which usually resolves in two to six weeks. Complete rest, possibly including bedrest is recommended for a short period of time, usually from one to three days. Nonsteroidal anti-inflammatory medication and heat (or ice) applied to the affected area are also commonly employed. Physical therapy is useful in many cases. Therapy may include gentle massage, ice and heat therapy, ultrasound, electrical muscle stimulation, and stretching exercises. Decompression therapy (traction) may also be utilized. Pain medication and muscle relaxants may also be beneficial in conjunction with the physical therapy.
Prognosis
The prognosis is excellent for a complete recovery from a lumbar strain or sprain injury. More than 90 percent of patients completely recover from an episode of lumbar muscle strain or sprain within one month. Heat and ice treatment are indicated on an "as needed" basis at home to treat sudden flare-ups of low back pain, along with anti-inflammatory medications.
Myelopathy
Myelopathy is a general term which describes the clinical presentation of a patient as a result of spinal cord pathology. The type of pathology can vary greatly, yet give rise to a very similar clinical presentation. When a patient develops myelopathy from cervical stenosis and spur formation it is termed a cervical spondylotic myelopathy. When the condition is due to a large cervical disc herniation causing compression of the cord and cervical stenosis it is termed a cervical discogenic myelopathy. Myelopathy can also be due to inflammatory or demyelinating disease (MS) and in this circumstance is termed a myelitis. Myelopathy that has it’s origin in vascular pathology is termed a vascular myelopathy. Myelopathy as a result of trauma is termed spinal cord injury. A patients exact presentation is partially dependent upon the underlying pathology, how chronic the compression has been, and the rate of progression of the compression.
The clinical presentation of myelopathy shares many of the symptoms and signs of spasticity - symptoms may include hypertonia (increased muscle tone), a loss of dexterity particularly seen in the hands, clonus (a series of rapid muscle contractions), exaggerated deep tendon reflexes, muscle spasms, scissoring (involuntary crossing of the legs), and urinary symptoms (frequency, urgency and incontinence). Myelopathy due to spinal cord compression is progressive until the compression is removed. Generally the patients’ neurologic status going into surgery will determine their surgical result- those patients with very advanced myelopathy have a much poorer prognosis than those individuals with a milder clinical presentation. For this reason early diagnosis and prompt treatment are recommended for individuals who have beed diagnosed with myelopathy from treatable causes.
Neck Pain
Your neck is the upper part of the spinal, the long flexible column which extends from your head to the lower aspect of your torso and gives support to the body. The cervical spine (neck region) consists of seven bones (C1-C7 vertebrae), which are separated from one another by intervertebral discs. These discs along with their supportive ligaments and joints allow the spine to move freely.
Age, injury, poor posture, or diseases such as arthritis can lead to degeneration of the bones or joints of the cervical spine, causing disc herniation or bone spurs to form,and lead to pain. Sudden severe injury to the neck may also contribute to disc herniation, “whiplash” (a term which describes severe sprain and strain of the neck muscles and ligaments), blood vessel injury, vertebral body fracture, and, in extreme cases, permanent paralysis. Herniated discs or bone spurs may cause a narrowing of the spinal canal and/or the foramina (small openings through which spinal nerve roots exit). Pressure on a nerve root by a herniated disc or a bone spur may result in pain involving the neck and/or numbness of the arms.
Pressure on the spinal cord in the cervical region can be a very serious problem which can cause severe numbness or weakness of the arms and legs, as well as progressive paralysis ( virtually all of the nerves to the rest of the body have to pass through the neck to reach their final destination).
Nonsurgical Treatment Options
Determining a treatment strategy depends mainly on identifying the exact location and cause of the neck and arm pain. Although neck pain can be quite debilitating and painful, nonsurgical management can alleviate many symptoms. Medications to reduce the pain or inflammation, muscle relaxants and gentle cervical traction may relieve symptoms while healing of the underlying condition takes place.
Physical therapy, massage therapy and occasionally steroid injections are also useful adjuncts to treatment. Conservative treatment options may continue for up to six or eight weeks.
Surgical Options
There are several surgical treatments available to treat cervical spine disorders. Factors that help determine the type of surgical treatment include the specifics of your disc disease, and the presence or absence of pressure on the spinal cord or spinal nerve roots, the distribution of the pain and the presence of spinal instability.
There are several different surgical procedures which can be utilized, the choice of which is influenced by the severity of your case.
If you smoke, you should quit. Smoking damages the structures and architecture of the spine and slows down the healing process. If you are overweight, you should lose weight. Both smoking and obesity have been shown to have a negative impact on spinal fusion surgery outcome.
Osteoathritis
Osteoarthritis is the most common type of arthritis, and affects middle-aged or older people more frequently. It can cause a breakdown of cartilage- the material that partially lines the articular surfaces of the joints- and can occur in almost any joint in the body. It most commonly affects the hips, knees, hands, lower back and neck.
When osteoarthritis affects the spine, it is known as spondylosis. Spondylosis is a degenerative disorder that can cause loss of normal spinal structure and function. Although aging is the primary cause, the rate of degeneration varies per person and may have a strong genetic influence. Obesity, joint overuse/abuse and previous injury to the affected area are also identified causes of spondylosis.
Spondylosis can affect the cervical, thoracic, and/or lumbar regions of the spine, with involvement of the intervertebral discs and facet joints. This can lead to disc degeneration, bone spurs, pinched nerves, and an enlargement or overgrowth of bone that narrows the central and nerve root canals, causing impaired function and pain. Patients usually complain of pain and stiffness, particularly in the morning upon rising from bed. Pain may be present as well, and increase in proportion to the amount and severity of activity undertaken throughout the day. Pain and stiffness may limit motion of the spine and be associated with pain, numbness and possibly weakness of the arms or legs.
A patient may develop spinal stenosis when spondylosis worsens. Spinal stenosis is a narrowing of spaces in the spine which results in pressure on the spinal cord and/or nerve roots. The narrowing can affect a small or large area of the spine. Pressure on the upper part of the spinal cord may produce pain or numbness in the shoulders and arms. Pressure on the lower part of the spinal cord or on nerve roots branching out from that area may cause pain or numbness in the legs.
A diagnosis can usually be made based on specific symptoms, a thorough physical examination, and x-ray results. On occasion, magnetic resonance imaging (MRI) may be ordered to determine the extent of damage in the spine. MRI can reveal damaged cartilage, loss of joint space, or bone spurs.
Nonsurgical treatment consists of the judicious use of anti-inflammatories, physical therapy and possibly steroid injections. Core strengthening and flexibility exercises and weight loss are useful in the management of this condition.
Surgery may be recommended if conservative treatment options, such as physical therapy and medications do not reduce or end the pain altogether, and the pain greatly impairs the person’s daily functions. The majority of surgery performed as a result of this condition is aimed t relieving spinal stenosis and its related symptoms.
Pinched Nerve
Pinched Nerve, or radiculopathy, is not a specific condition, but rather a description of a problem in which one or more nerves are affected by various disease processes. This can result in pain (radicular pain), weakness, numbness, or difficulty controlling specific muscles.
In a radiculopathy, the problem is at or near the root of the nerve, along the spine. However, the pain or other symptoms may manifest in an extremity through a process called referred pain. For example, a nerve root impingement in the neck can produce pain and weakness in the forearm.
Polyradiculopathy is the name of the term for describing more than one spinal nerve root is affected by a disease process.
The nerve or nerves that are "pinched" may be inflamed, compressed by various lesions (herniated disc, spur), lack blood flow, or may be affected by a disease that is destroying the nerve root in part or totally.
Sciatica
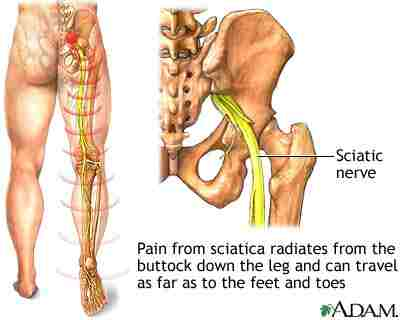
Sciatica is a set of symptoms which includes pain that may be caused by compression and/or irritation of the nerve roots that give rise to the sciatic nerve, or by compression or irritation of the sciatic nerve itself. The pain is felt in the lower back, buttock, and/or various parts of the leg and foot. In addition to pain, which is often severe, there may be numbness, muscular weakness, and difficulty in moving or controlling the leg. Typically, the symptoms are only felt on one side of the body.
Although sciatica is a relatively common form of low back pain and leg pain, the true meaning of the term is often misunderstood. Sciatica is a set of symptoms rather than a diagnosis for what is irritating the root of the nerve, causing the pain. This point is important, because treatment for sciatica or sciatic symptoms will often be different, depending upon the underlying cause of the symptoms.
Because of the many conditions which can compress nerve roots and cause sciatica, the exact symptoms often differ from patient to patient. Diagnostic tests therefore need to be tailored to the patients presentation and includes a physical exam which includes both a neurological exam and a mechanical exam. Patients are often asked to adopt numerous positions and actions such as squatting, walking on toes, bending forward and backward, rotating the spine, sitting, lying on back, and raising one leg at a time. The physician will assess the patient ability to carry out these activities in combination with the findings of the neurological exam.
The results of this evaluation will indicate what additional diagnostic tests are required. These tests often include radiology exams such as spinal Xrays, CT scans and MRI scans. Electrophysiologic testing such as nerve conduction EMG may also be indicated.
TREATMENTS
Treatment of the underlying cause of the compression is the most effective course. When the cause is due to a prolapsed or lumbar disc herniation, research has shown that, with conservative care ( rest, ant inflammatories, muscle relaxants, narcotic pain relievers, physical therapy, injections, etc.) 75% of patients with disc herniations causing sciatica will experience resolution of their pain with time. In patient whom conservative care has not allowed amelioration of their symptoms, surgery can allow relief of these symptoms.
Lumbar microdiscectomy or minimally invasive lumbar discectomy are surgical good options that offer relief of these symptoms.
Spasticity
Spasticity is a disorder of the central nervous system which expresses itself as increased muscle tone and an abnormal contraction of opposing muscle groups. This condition can make tasks such as walking very difficult and sometimes impossible.
Voluntary movement is controlled by several interacting systems within the nervous system. Primary control is through the upper motor neurons of the motor cortex of the brain, which send their axons via the cortico-spinal tracts to connect to lower motor neurons in the spinal cord. Spasticity is caused by damage to upper motor neurons or to the cortico-spinal tracts. This damage may occur as a consequence of spinal cord injury, syrinx, multiple sclerosis, cerebral palsy, anoxic brain damage, traumatic brain injury, spinal fractures , cervical stenosis and thoracic stenosis.
Symptoms may include hypertonia (increased muscle tone), a loss of dexterity particularly seen in the hands, clonus (a series of rapid muscle contractions), exaggerated deep tendon reflexes, muscle spasms, scissoring (involuntary crossing of the legs), and and urinary symptoms (frequency, urgency and incontinence).
The degree of spasticity varies from mild muscle stiffness to severe, painful, and uncontrollable muscle spasms. Cold weather, fatigue and multi-tasking may trigger more severe spasms. The condition can interfere with daily activities. Over the years, the symptoms may increase in severity, depending on the underlying condition causing the spasticity.
Spinal Cord Injury
Spinal cord injury causes damage to the cell bodies and myelinated fiber tracts of the spinal cord that carry sensation and motor signals to and from the brain.
The clinical effects of a spinal cord injury vary according to the type and level of injury, and can be organized into several types. In a “complete” injury, the spinal cord is injured to the point where it has complete cessation of function at the level of injury. This rarely is due to transection of the spinal cord. At the level of injury the pathological findings of contusion (bruising), infarction (stroke), swelling and hemorrhage are often found. Some cells may survive and some fibers may still be intact but cannot function at that time due to the extent of injury. Therefore there is no function below the injured level and the patient is said to have a "complete" spinal cord injury. Current research is directed towards understanding the inflammatory mediators of spinal cord injury, limiting the secondary damage to the cord by inflammation and swelling and developing neuroprotective/reparative medications to help the recovery of the damaged tissue.
In an “incomplete” injury, the patient retains some sensation or movement below the level of the injury. The severity of the spinal cord injuries in the incomplete category vary, and are described clinically using the ASIA scale. Recent evidence suggest that over 95% of people with "incomplete" spinal cord injury recover some locomotory ability.
A special form of incomplete spinal cord injury is seen in the setting of cervical stenosis, and is termed central cord syndrome. This spinal cord injury usually comes about when a patient with cervical spinal stenosis suffers a hyperextension injury to the cervical spine. These individuals present with weakness of the upper extremities, especially the hands, more so than the legs. There i usually profound numbness and tingling of the hands, and the numbness may have an electric burning type quality termed dysesthesia. Bowel and bladder dysfunction may also be seen.
Spinal Fracture/Vertabral Fracture
A Spinal Fracture is a medical condition in which a vertebral body is cracked, burst or compressed. While many fractures are the result of high force impact or stress, bone fracture can also occur as a result of certain medical conditions that weaken the bones such as osteoporosis, certain types of cancer, or osteogenesis imperfecta.
Falls and motor vehicle accidents are the two most common causes of spinal fracture. Many of these injuries will never require surgery, but major fractures can result in serious long-term problems unless treated promptly and properly. There are a variety of types of spine fractures, ranging from severe injuries such as burst fractures and fracture-dislocations (usually caused by severe trauma) to painful compression fractures, often a result of more minor trauma in osteoporotic patients. Depending on the segment of spine fractured, these injuries can result in pain and spinal cord injury.
SYMPTOMS
Almost always the patient complains of severe pain over the segment of spine which is fractured. The pain is usually worsened with movement and weight bearing. Because the spinal cord and nerve roots are contained within the spinal canal, these structures may also be injured by compression or distortion which occurred during the injury or as a result of the displaced bone fragments. This may result in a loss of sensation, weakness or paralysis. Indications of nerve compression or injury include pain radiating into the arm or leg, weakness of the arm or leg muscles, and incontinence.
TREATMENTS
Treatment is dependent on the location of the fracture on the vertebral body itself, the severity of the distortion of the vertebral body, the amount of resultant instability of the spine and the severity of the patients pain. Many fractures may be treated effectively by bedrest and bracing. Other more serious fractures may require surgery.
Spinal fusion surgery is a highly specialized procedure which requires a thorough understanding of the mechanics of spinal injuries, and training in the evolving techniques for reconstructing the spinal column. The exact procedure performed depends on the degree of spinal fracture, the degree of deformity of the spinal column, the degree of instability of the spinal column and if there exists compression of the spinal cord and nerve roots. In the case of vertebral compression fractures, spinal surgeons can perform kyphoplasty/vertebroplasty to re-expand the vertebrae and reinforce the fractured bone with an injection of bone cement. This can be done as an outpatient procedure in a minimally invasive fashion.
Spinal Instability
Spinal Instability is the inability of the spinal column to maintain its normal configuration under normal conditions. The function of the spine is to provide structure, protection, and support for the body and its internal organs. In an unstable spine, the integrity of the spine is compromised such that it is no longer able to provide these essential functions. This condition may be caused by congenital defects, trauma, degenerative changes, or neoplastic diseases affecting the spine (the vertebrae, intervertebral discs, or spinal ligaments).
SYMPTOMS
The symptoms of lumbar spinal instability are often similar to sciatica often a deep, severe pain that starts in the affected area of the spine and then shoots down the buttock and the leg with certain movements. The pain can be most severe after prolonged sitting and standing, on standing from a low seated position, or with bending, twisting and lifting. Coughing, sneezing or laughing may exacerbate the pain. Pain may also be accompanied by weakness of the leg or foot. Movement can also trigger extremely painful muscle spasms, particularly if the spinal column is tilted fore or aft of it neutral position.
TREATMENTS
There is a broad spectrum of appropriate treatments for this condition , depending on the severity and cause of the symptoms.
As part of the normal aging process, many people experience the loss of some amount of spinal integrity due to conditions such as spinal arthritis or degenerative disc disease. Mild asymptomatic cases of instability may not require intervention, or may be relieved through physical therapy to build up surrounding core and spinal muscles to help stabilize the spinal column and prevent pain.
Congenital instability or instability caused by trauma often require surgical treatment. Some form of surgical fusion of the spine can often repair the instability. Many procedures have been developed to address the various causes of instability, including microneurosurgical and minimally invasive techniques. As spinal instability is a generalized term, it includes many specific types of physical issues, and thus there are different approaches to their treatment. Thorough examination and evaluation of the patient, including an appropriate radiological workup is required for accurate understanding and diagnosis of the underlying problem. The results of this evaluation dictate the specific surgical remedy when indicated.
Spinal Stenosis
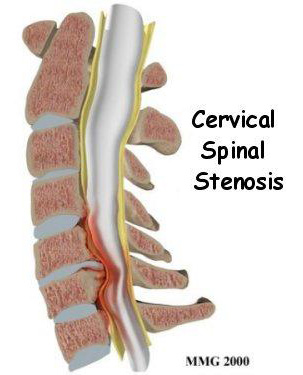 Spinal stenosis is a medical condition in which the spinal canal narrows and compresses the spinal cord and/or spinal nerves. This is usually due to the natural process of spinal degeneration that occurs with aging. It can also sometimes be caused by spinal disc herniation, osteoporosis, or tumor. Spinal stenosis may affect any part of the spine, including the cervical, thoracic or lumbar segments.
Spinal stenosis is a medical condition in which the spinal canal narrows and compresses the spinal cord and/or spinal nerves. This is usually due to the natural process of spinal degeneration that occurs with aging. It can also sometimes be caused by spinal disc herniation, osteoporosis, or tumor. Spinal stenosis may affect any part of the spine, including the cervical, thoracic or lumbar segments.
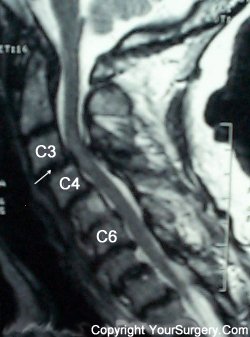
The main causes of cervical spinal stenosis include cervical spondylosis(arthritis), diffuse idiopathic skeletal hyperostosis (DISH) , or ossification of the posterior longitudinal ligament (OPLL).
Cervical spinal stenosis is more common in males than females, and is mainly found in the 40-60 year age group.
Signs of cervical spinal stenosis include spastic gait; upper or lower extremity numbness; upper extremity or lower extremity weakness; radicular pain involving the arms; sphincter disturbances; muscle wasting; sensory deficits; and reflex abnormalities. This clinical symptom complex is termed myelopathy.
Lumbar spinal stenosis results in low back pain as well as pain or abnormal sensations involving the legs. Often patients complain of a severe limitation in their ability to walk any distance, or stand for any significant length of time. This clinical symptom complex is termed neurogenic claudication. In this instance, patients find that if they sit for a period of time, the symptoms abate and they can continue to walk an additional short distance. Some patients have reported bending over at the waist while standing in an effort to relieve their symptoms, which places the lumbar spine in a flexed position similar to sitting. Another common remark from patient with this condition is the ability to ambulate much farther if they can lean on a shopping cart- the so called “shopping cart sign” because of its reliability in indicating this spinal condition.
TREATMENTS
Treatment is dependent upon the segment of the spine involved. In the circumstance of cervical or
thoracic spinal stenosis, the spinal cord itself is compressed. The spinal cord is very sensitive to compression and in the patient who has developed signs and symptoms of
myelopathy(see above) the spinal cord is being damaged. There is little role for conservative treatment in this situation, since the condition of myelopathy is usually progressive, due to more and more spinal cord injury. Treatment therefore is usually surgical decompression of the spinal cord. Depending on the cause of the spinal cord compression, surgical treatment may include a
cervical decompressive laminectomy
or an
anterior cervical discectomy and fusion.
Treatment of lumbar stenosis on the other hand is often conservative, and includes physical therapy, anti inflammatories, weight loss, and core stabilization exercises. Epidural steroid injections may also help relieve the leg pain. Research has indicated that approximately 50% of individuals suffering from lumbar spinal stenosis will experience symptomatic relief with these measures, thereby avoiding surgery
If the symptoms are more severe, or accompanied by significant neurological compromise, a lumbar decompressive laminectomy and foraminotomy may be indicated to relieve pressure from the lumbar spinal nerve roots.
Recent developments include several new implants used in surgery to treat the symptoms of spinal stenosis, while preserving the lumbar lamina, thus avoiding laminectomy. Spinal implants such as the X STOP, work by indirect decompression, called Interspinous Process Decompression.
Spinal Tumors
Although the majority of back pain is due to degenerative conditions of the spine, rarely the cause may be a spinal tumor. These growths may be cancerous or noncancerous that develop in spinal cord or nerve roots, the meninges (covering of the cord and nerve roots), or in the skeletal structure of the spine. These tumors may develop primarily from these structures, or may be metastatic- i.e. come from another tissue of the body.
Metastatic tumors metastasize (spread) via arteries, veins, lymphatic system, and by direct invasion. Malignant tumors of the breast, prostate, lung, gastrointestinal tract and kidney can spread into the spine.
Regardless of the origin of the tumor, spine tumors may cause problems by compression of the spinal canal, possibly leading to paralysis or other neurologic dysfunction. As a spinal tumor grows, it can affect the spinal cord, blood vessels, meninges, nerve roots, or the bones of the spine.
SYMPTOMS
Back pain is often the primary symptom. The pain may or may not be related to activity. It can occur either while moving or while at rest, and is sometimes noted to be worse at night. Other symptoms are determined by what structures are involved with the tumor other that the bony vertebrae. If the spinal cord or nerve roots are compressed by the tumor there are often symptoms of numbness, sciatica, weakness or partial paralysis of the limbs, or loss of bowel/bladder control. Destruction of the supporting elements of the spine may lead to spinal deformity (such as kyphosis or scoliosis).
TREATMENTS
Recent advances in treating spinal tumors offer various treatment options, including various types of surgical techniques. Depending on the nature of the tumor, additional treatment in the form of chemotherapy and/or radiation therapy may be indicated.
Spondylotithesis
Spondylolithesis is the spinal malalignment that occurs when one vertebra slips forward on it’s neighboring vertebra. The slip is always forwards, or towards the belly if the term spondylolithesis is used. If the vertebra sips to the side, or if it slips backwards the term subluxation is used instead.
Spondylolithesis may occur due to a congenital or acquired crack in a part of the lamina called the pars interarticularis. This portion of the lamina connects the facet joints that engage the vertebra below, thereby controlling translation (forward slip) of that vertebra. In the event these joints are broken off, the vertebra may move forward. The other common cause of spondylolithesis is advanced degenerative change of both the intervertebral disc and the facet joints at a given level. Usually the patient has a degree of osteopenia or osteoporosis as well. The slip occurs in this instance due to the increased movement of the degenerated disc combined with degeneration and distortion of the facet joints. The combination allows the forward slip.
Patients with symptomatic spondylolithesis often complain of back pain as well as leg pain. The back pain is usually exacerbated by standing, walking and bending. Leaning forward, twisting at the waist and carrying objects also increase back pain. Since the malalignment of the vertebrae often leads to lumbar spinal stenosis, the patients may also have the symptom of neurogenic claudication.
Bilateral leg pain and severe ambulatory dysfunction are common issues in these patients.
Treatment options are tailored to the cause and severity of the spondylolithesis, but in general a course of conservative care is carried out. This treatment includes physical therapy, anti inflammatories, weight loss, and core stabilization exercises. Epidural steroid injections may also help relieve the leg pain. Other injections, including those of the facet joints and the pars interarticularis may also be considered. A trial of lumbar bracing and/or decompression therapy may also be undertaken.
In those patients who fail conservative care, the varied surgical options may be explored. Because there exists spinal instability and spinal stenosis in these patients, often lumbar spinal fusion and lumbar decompressive laminectomy are considered.
Syringomyelia
Syringomyelia is a generic term referring to a disorder in which a cyst or tubular cavity forms within the spinal cord. This cyst, called a syrinx, can expand and elongate over time, destroying the spinal cord. Since the spinal cord connects the brain to nerves in the extremities, this damage may result in pain, weakness and loss of sensation affecting the back, shoulders, arms, legs, bowel and bladder. Other symptoms may include headaches and neck pain, as well as a loss of the ability to feel extremes of hot or cold, especially in the hands. Each patient experiences a different combination of symptoms. These symptoms typically vary depending on the extent and, often more critically, on the location of the syrinx within the spinal cord.
Other, more common disorders share the early symptoms of syringomyelia. In the past, this has made diagnosis difficult. The advent of magnetic resonance imaging or MRI, has significantly increased the number of syringomyelia cases diagnosed in the beginning stages of the disorder.
Syringomyelia has a prevalence estimated at 8.4 cases per 100,000 people, or about 21,000 Americans, with symptoms usually begin in young adulthood. Signs of the disorder tend to develop slowly, although sudden onset may occur with coughing, straining, or myelopathy. If not treated surgically, syringomyelia can lead to progressive weakness of the arms and legs, loss of hand sensation, and chronic, severe pain.
Syringomyelia is often associated with, and the result of a condition called Chiari malformation (Arnold-Chiari malformation). In this condition, a portion of the cerebellum prolapses into the upper cervical spinal canal, causing abnormal CSF flow.
SYMPTOMS
Syringomyelia causes a wide variety of neuropathic symptoms due to damage of the spinal cord. Patients may experience chronic pain, abnormal sensations and loss of sensation particularly in the hands. Some patients experience paralysis or paresis temporarily or permanently. A syrinx may also cause disruptions in the parasympathetic and sympathetic nervous systems, leading to abnormal body temperature or sweating, bowel control issues, or other problems. If the syrinx is higher up in the spinal cord or affecting the brainstem as in syringobulbia, vocal cord paralysis, ipsilateral tongue wasting, trigeminal nerve sensory loss, and other signs may occur.
TREATMENTS
Physicians now use magnetic resonance imaging (MRI) to diagnose syringomyelia. The MRI scanner produces images of body structures, such as the brain and spinal cord, in vivid detail. This test can demonstrate the syrinx in the spinal cord, and allows the physician to evaluate the patient for other conditions which may mimick the symptoms of syrinx, such as the presence of a tumor. MRI is safe, painless, and informative and has greatly improved the diagnosis of syringomyelia.
The first step after diagnosis is finding a neurosurgeon who is experienced in the treatment of syringomyelia. Surgery is the only viable treatment for syringomyelia, and a neurosurgeon is the only specialist qualified to provide a fully informed recommendation. Not all patients will advance to the stage where surgery is needed. Evaluation of the condition is often difficult because syringomyelia can remain stationary for long periods of time, however in some cases may progress rapidly.
Vertebral Compression Fractures
Incidence and Prevalence
An estimated 10 million Americans have osteoporosis, and an additional 34 million are estimated to have low bone mass, placing them at increased risk for developing this condition. The majority of the 10 million Americans with osteoporosis are women.
Vertebral compression fractures (VCFs) are the most common fracture in patients with osteoporosis, affecting about 750,000 people annually. VCFs affect an estimated 25 percent of all postmenopausal women in the United States. The prevalence of this condition steadily increases as people age, with an estimated 40 percent of women age 80 and older affected. Although far more common in women, VCFs are also a major health concern for older men.
People who have sustained one osteoporotic VCF are at five times the risk of sustaining a second VCF. Occasionally a VCF can be present with either minor symptoms or no symptoms, but the risk still exists for additional VCFs to occur.
Causes
VCFs occur when the bony block or vertebral body in the spine collapses, which can lead to severe pain, deformity and loss of height. These fractures more commonly occur in the thoracic spine (the middle portion of the spine), especially in the lower part. While osteoporosis is the most common cause, these fractures may also be caused by trauma or metastatic tumors. In people with severe osteoporosis, a VCF may be caused by simple daily activities, such as stepping out of the shower, sneezing vigorously or lifting a light object.
Metastatic tumors should be considered as the cause in patients younger than 55 with no history of trauma or only minimal trauma. The bones of the spine are a common place for many types of cancers to spread. The cancer may cause destruction of part of the vertebra, weakening the bone until it collapses.
The main clinical symptoms of VCFs may include the sudden onset of back pain which increases with weight bearing, and decreases with the supine position. Focal point tenderness over the fracture is also characteristic.
When a fracture leads to a vertebral body collapse of more than 50 percent, there is a risk of segmental instability. The spinal segments work together to enable weight bearing, movement, and support of the entire spine. When one segment deteriorates or collapses to the point of instability, it can produce pain and impair daily activities. The instability ultimately results in quicker degeneration of the spine in the affected area.
Kyphosis is a common disorder in older women who have osteoporosis and frequent VCFs. The front of the vertebrae will collapse and "wedge" due to the lack of normal vertebral space. Kyphosis leads to a more rounded thoracic spine. This deformity is sometimes referred to as hunchback or dowager’s hump.
Severe kyphosis may cause extreme and debilitating pain. The hunchback deformity may eventually compress the heart, lungs, and intestines. This in turn can lead to fatigue, shortness of breath, and loss of appetite.
If the fracture causes part of the vertebral body to place pressure on the spinal cord, the nerves and spinal cord can be affected. The normal space between the spinal cord and beginning of the spinal canal can be reduced if pieces of the broken vertebral body push into the spinal canal.
The narrowing of the spinal canal due to a VCF can lead to immediate injury to the spinal nerves, or can cause problems later from irritation of the nerves. The lack of space can also lower the supply of blood and oxygen to the spinal cord. This can lead to numbness and pain in the nerves that are affected. The nerves may lose some of their mobility when the space around them decreases, which can lead to nerve irritation and inflammation.
Diagnosis
While a diagnosis can usually be made through history and a physical examination, plain x-rays, computed tomography or magnetic resonance imaging, can help in confirming diagnosis, predicting prognosis, and determining the best treatment option for the patient.
Nonsurgical Treatment
Traditionally, people with severe pain from VCFs have been treated with bed rest, medications, bracing, or invasive spinal surgery, often with limited effectiveness. Pain secondary to acute vertebral fracture appears to be caused in part by vertebral instability (nonunion or slow-forming union) at the fracture site. VCF-related pain that is allowed to heal naturally can last as long as three months. However, the pain usually decreases significantly in a matter of days or weeks.
Bed rest may be advised for a short period of time, followed by a limitation on some activities. However, prolonged inactivity should be avoided.
Over-the-counter pain medications are often effective in relieving pain. Both acetaminophen and non-steroidal anti-inflammatory drugs (NSAIDs) are commonly recommended. Narcotic pain medications and muscle relaxants are often prescribed, but only for short periods of time, due to the risk of addiction.
Back bracing can provide external support to limit the motion of fractured vertebrae, similar to the support a cast provides on a leg fracture. The rigid style of back brace limits spine-related motion greatly, which may help reduce pain.
While immediate treatment is essential to alleviating the pain and risks of the fracture, prevention of subsequent fractures is very important. Daily intake of adequate amounts of Vitamin D3 and calcium are very important. In addition,bone-strengthening drugs known as bisphosphonates (i.e.: Actonel, Boniva, and Fosamax) may be prescribed to help stabilize or restore bone loss.
When conservative treatment options have proven ineffective, two minimally invasive procedures, called vertebroplasty and kyphoplasty may be considered as treatment options. Recent advances in spinal procedures have reduced the need for invasive surgery, in many cases.
Vertebroplasty for the treatment of VCFs was introduced in the United States in the early 1990s. The procedure is usually done on an outpatient basis, although some patients stay in the hospital overnight. The procedure may be performed with a local anesthetic and intravenous sedation or general anesthesia. Using x-ray guidance, a small needle containing specially formulated acrylic bone cement is injected into the collapsed vertebra. The cement hardens within minutes, strengthening and stabilizing the fractured vertebra. Most experts believe that pain relief is achieved through mechanical support and stability provided by the bone cement.
A newer procedure, called kyphoplasty, involves the creation of a cavity within the fractured vertebra before the cement is injected into the vertebra. The cavity may be created by a variety of mechanical methods, and allows the viscosity (thickness) of the cement injected to be quite high. This allows the procedure to be safer, since the cement may be more readily controlled, and has the potential to restore some of the lost vertebral height.